A strange and deadly trend called bluetoothing is spreading quietly across parts of Africa. It sounds like a phone feature, but in this case, it has nothing to do with technology. Bluetoothing is a risky way some people try to share drugs by injecting each other’s blood , this is to enable them get cheaper source of highness as they can not afford the drugs themself— and this it’s putting many lives in danger.
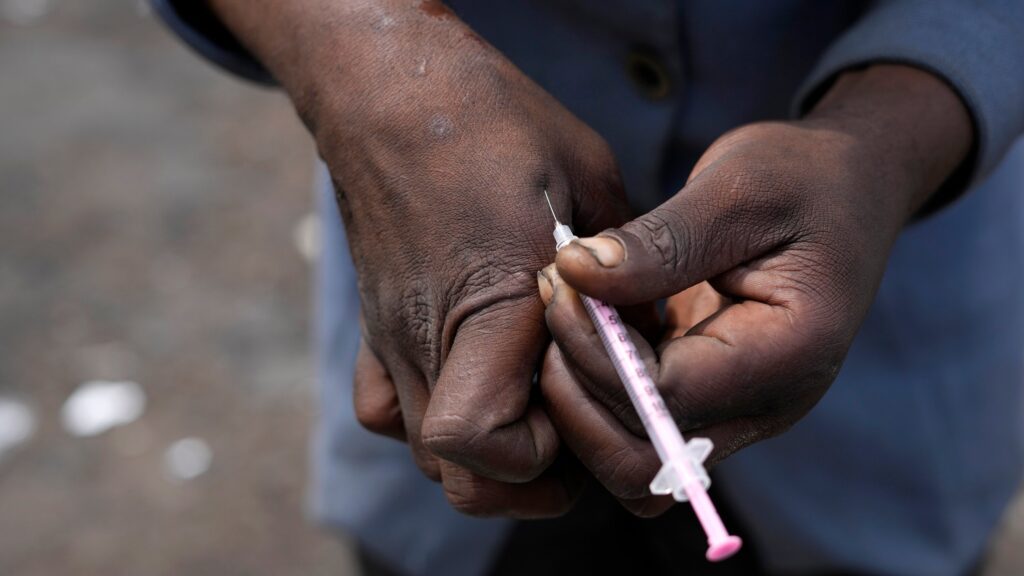
What is bluetoothing and how did it start?
Bluetoothing, also known as flash-blooding, began more than a decade ago in East Africa, especially among people struggling with heroin addiction in Tanzania. The idea spread to South Africa and other countries, and today reports show it’s also happening in Lesotho and other parts of southern Africa.
Here’s what happens:
One person injects a drug, usually heroin or methamphetamine. Right after that, they draw some of their own blood into the same syringe, believing the drug is still in their bloodstream. They then pass that syringe of blood to someone else, who injects it to get “the same high” without using more drugs.
People often do this because drugs are expensive or hard to find. But the truth is, this method doesn’t really work — and it comes with deadly risks.
Why bluetoothing is so dangerous
Doctors and health experts say bluetoothing is one of the most dangerous drug habits seen in recent years. It exposes people to a long list of deadly infections and medical problems.
1. High risk of HIV and hepatitis transmission
When people inject someone else’s blood, they are directly injecting any virus or infection that person has. This makes the spread of HIV, hepatitis B, and hepatitis C extremely likely. A recent South African study found that almost one in five people who inject drugs admitted to bluetoothing, and more than a third were living with HIV.
Even worse, in most cases the same syringe and needle are reused, multiplying the chance of infection. As one health expert put it, bluetoothing is “the perfect way to spread HIV.”
2. It doesn’t actually get you high
Many users believe they can get “two highs for the price of one.” But scientists say the amount of drug that remains in blood after injection is tiny — not enough to create any real effect. The feeling people describe is often psychological, not chemical.
3. It spreads beyond drug users
The danger doesn’t stop with drug users. Once a person becomes infected with HIV or hepatitis, the virus can easily spread to sexual partners, unborn babies, or anyone exposed to infected blood. That means bluetoothing can quietly worsen national HIV epidemics even outside drug-using communities.
4. Other infections and organ damage
Injecting someone else’s blood can also spread dangerous bacteria, leading to sepsis (blood poisoning), endocarditis (heart infection), or abscesses. Many victims end up in hospitals with serious liver or kidney damage.
Why people do it anyway

Most people who engage in bluetoothing are not doing it for fun. They often live in poverty, with little access to addiction treatment or clean needles. Some are homeless or unemployed, struggling to survive. Because drugs are costly, people share blood as a way to “stretch” the drug supply.
In Lesotho, mothers have formed groups to fight against bluetoothing and educate young people about its dangers. Many say they lost children or relatives to this deadly trend.
What health workers can do
Health workers across Africa are being urged to ask patients about blood-sharing and injection practices, especially in communities where drug use is common. Because many people hide or deny this behaviour out of shame, it’s easy for doctors to miss.
Experts recommend several key steps:
- Offer free or affordable HIV and hepatitis testing to anyone who injects drugs.
- Provide clean syringes, safe disposal points, and drug-substitution therapy like methadone to reduce injection risk.
- Educate communities about the dangers of injecting blood and how infections spread.
- Treat those who test positive quickly and link them to ongoing care.
- Introduce Needle exchange programs
Studies show that when people who inject drugs are supported with medical help, counselling, and harm-reduction services, infection rates drop dramatically.
Why bluetoothing matters now
African countries have made real progress in fighting HIV and hepatitis, but bluetoothing threatens to reverse those gains. The practice is spreading quietly among young people, especially in areas with high unemployment, drug shortages, and limited health services.
Without quick action — awareness campaigns, addiction support, and harm-reduction programs — this trend could fuel a new wave of infections across communities already under strain.
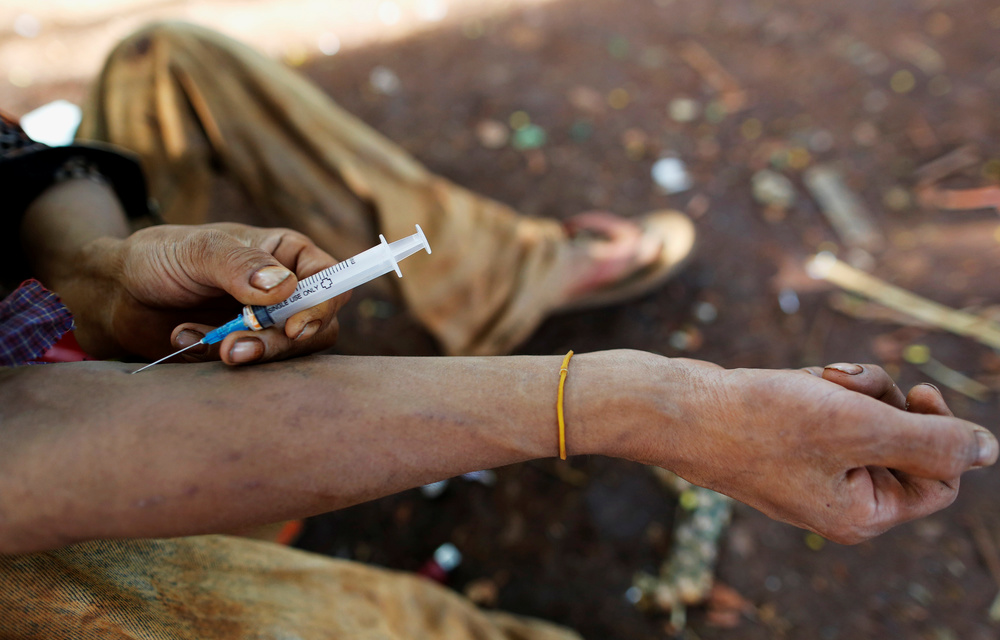
Bluetoothing may sound like a shortcut to a cheaper high, but it’s really a shortcut to infection and death. Sharing blood is not just unsafe — it’s one of the fastest ways to spread HIV and hepatitis. There is no safe version of this practice. The only real protection is awareness, clean needles, addiction treatment, and access to healthcare.
If you or someone you know is injecting drugs, seek help from a health clinic or harm-reduction center. Modern treatment options like methadone therapy can manage addiction safely and effectively — no blood sharing required.
