Across hospitals and clinics in Africa, health workers are facing tougher days. Doctors and nurses are doing their best with very limited resources. Mothers still walk long distances to get medical care, and public health workers juggle many urgent tasks at once—often without the tools they need.
This is the reality for more than 1.4 billion Africans, as global funding for health slowly declines.
Many African governments are trying hard to spend more on health, but the money available still falls short of what’s needed to deliver basic services or build stronger, more reliable health systems. At the same time, donor funding is flattening, and humanitarian needs are rising. The safety net that once supported health progress is getting thinner.
Africa holds over one-sixth of the world’s population, but carries almost a quarter of the global disease burden. That imbalance tells us something urgent must change—but it also hides a story of hope and determination.
Africa Is Rising: Ingenuity and Self-Determination in Action
Despite challenges, African countries are proving what can be achieved with creativity and unity.
At the World Health Organization (WHO) Regional Office for Africa, efforts are focused on helping countries take charge of their own health future—by building local talent, preparing for future health threats, and focusing on practical solutions that last.
The progress is real. During outbreaks, it used to take weeks to deliver supplies. Now it takes just 72 hours. Detecting new outbreaks has also become much faster—cutting response times from 14 days in 2017 to just 3 days in 2024.
When COVID-19 hit, African countries showed their ability to innovate under pressure. Many used existing GeneXpert machines—originally for tuberculosis testing—to conduct quick and affordable COVID tests. Local businesses started producing masks, sanitizers, and even ventilators at lower costs. Countries like Rwanda led the way with home-grown health technologies.
And it’s not only COVID. Countries such as Rwanda, The Gambia, Mauritania, Zimbabwe, and Liberia have made strong gains against malaria, using community health workers, free mosquito nets, and smart use of data. In 2024, Cabo Verde became officially malaria-free—proof that success is possible even with limited resources.
Other countries are celebrating major milestones too.
- Guinea eliminated sleeping sickness (Human African Trypanosomiasis).
- Niger ended river blindness (Onchocerciasis).
- Mauritania, Burundi, and Senegal wiped out Trachoma.
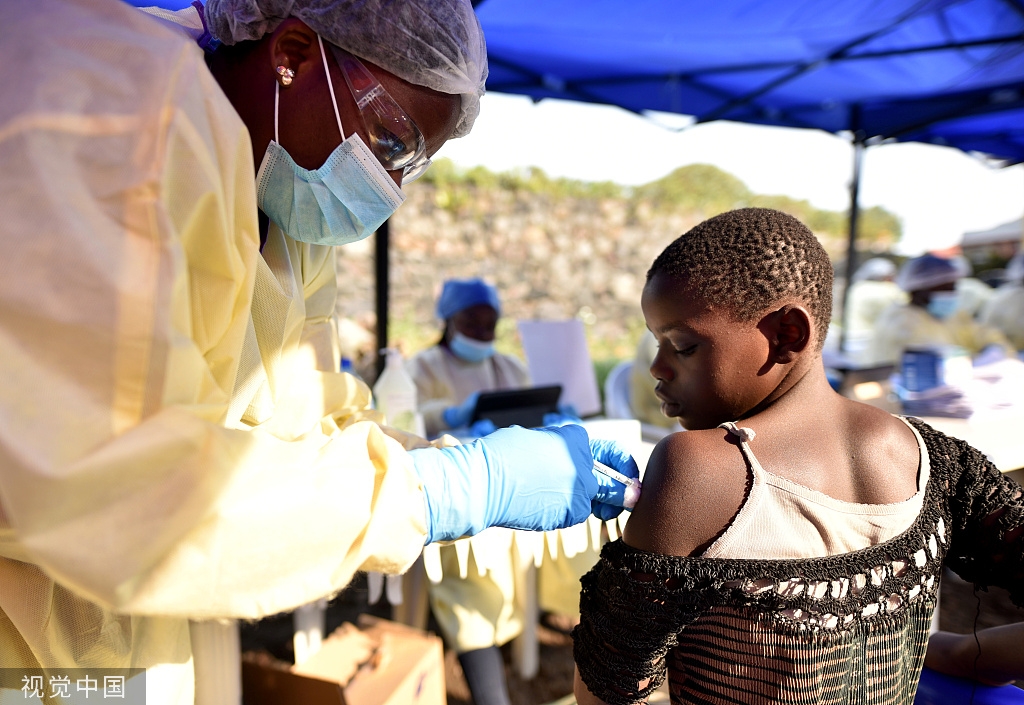
These wins show what can happen when countries take ownership and stay committed.
Universal Health Coverage: Health Care for Everyone
Good health should not be a privilege. But today, more than 400 million Africans still cannot access basic health services. Behind those numbers are real people—mothers giving birth without skilled care, children missing vaccines, and elderly people living without treatment.
Universal Health Coverage (UHC) means ensuring everyone can access care without financial hardship. It starts with strong primary health care close to home.
That means:
- Training and supporting community health workers.
- Improving maternal and child health services.
- Using digital tools to make care faster and more efficient.
- Making health care affordable and accessible to all.
These investments don’t just save lives—they secure the future for generations to come.
Building Resilience: Preparing for Tomorrow’s Crises
COVID-19 reminded the world that health systems must be ready for anything. But Africa has always faced recurring challenges—disease outbreaks, floods, droughts, and conflicts.
Resilience means planning ahead, not just reacting. It means:
- Factoring climate change into health planning.
- Combating antimicrobial resistance (when medicines stop working).
- Adopting the One Health approach, which recognizes the link between human, animal, and environmental health.
- Strengthening disease surveillance and emergency preparedness.
A resilient health system is one that can adapt, respond, and recover—faster and stronger each time.
Efficiency and Modernization: Making Every Dollar Count
When money is tight, every coin matters. Efficiency isn’t about cutting costs—it’s about getting the most value out of every investment.
Countries are modernizing how health care works—using digital tools, smarter supply chains, and data-driven decisions. Kenya’s e-health systems and Nigeria’s vaccine-tracking technology are great examples.
By sharing lessons and innovations across borders, countries can do more with less—without lowering the quality of care.
Health Sovereignty: Africa Taking the Lead
Africa’s health future should be driven by Africans. That means being able to produce our own vaccines, medicines, and medical supplies, and to fund and lead our own health priorities.
The pandemic exposed how dangerous it is to rely too heavily on others for essential supplies. Now, countries like Egypt, Nigeria, and South Africa are investing in local vaccine manufacturing and stronger regulatory systems.
The WHO is helping countries build the African Medicines Agency, which will ensure safer, high-quality products across the continent.
Health sovereignty is not just about pride—it’s about having the power to protect lives without waiting for outside help.
A Call to Partners: Don’t Step Back—Step Up
Global health funding may be shrinking, but this is not the time to give up. It’s the time to invest smarter and support what’s working.
Africa is not waiting for rescue—it’s building solutions from within. But international partnerships still matter. Donors and global institutions should focus on locally led projects, sustainable systems, and long-term results.
