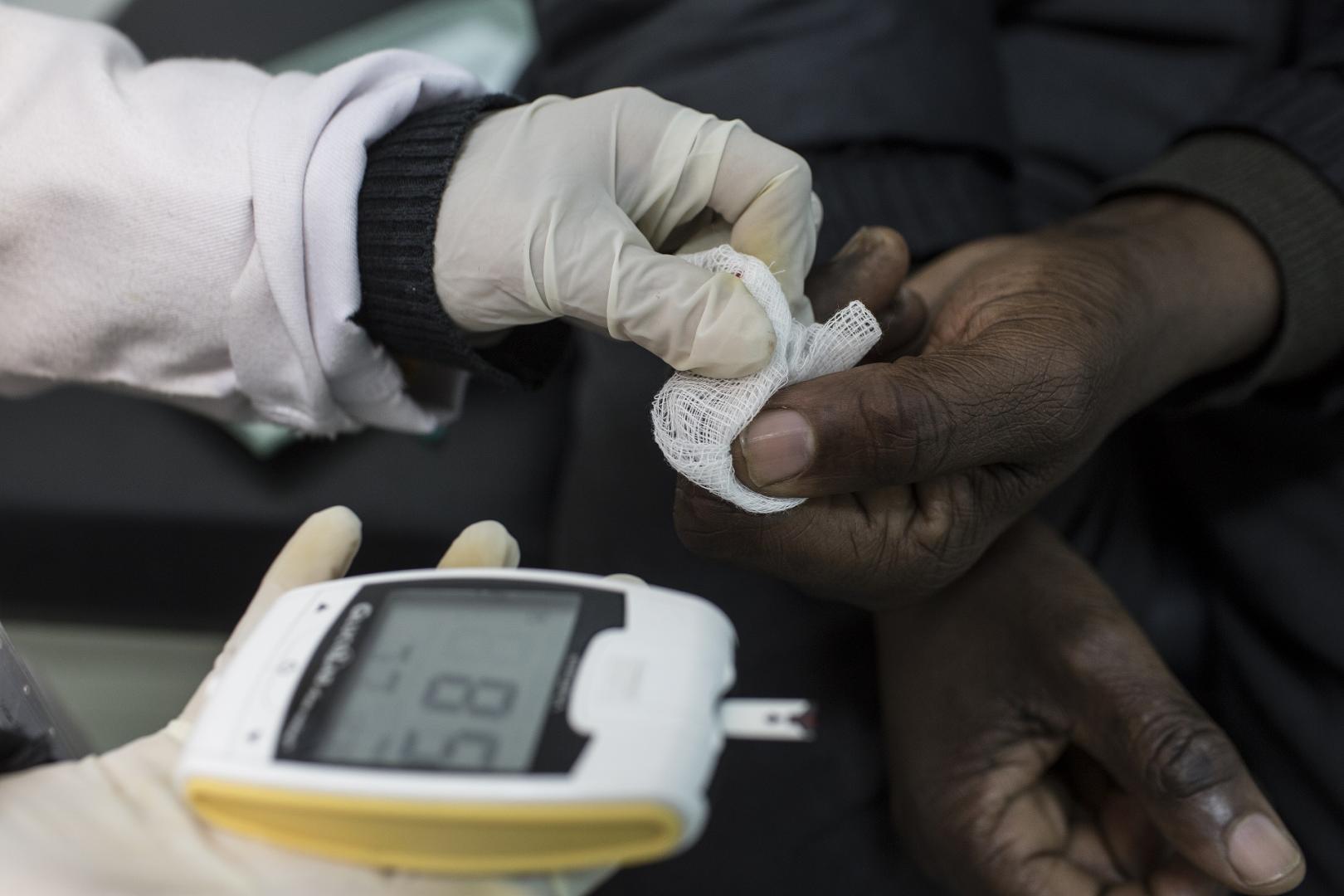
Diabetes mellitus is rapidly becoming one of the most pressing non-communicable disease issues in Africa. With rates climbing, many in sub-Saharan Africa continue to live with undiagnosed or untreated disease, increasing their risk of serious complications such as cardiovascular disease, kidney failure, and vision loss. To better support patients, health authorities, and practitioners, it is essential to understand what diabetes is, how it manifests in African populations, how it is diagnosed and managed, and the strategies needed for long-term improvement.
What Is Diabetes Mellitus?
Diabetes mellitus is a chronic metabolic disease defined by persistently elevated blood glucose (sugar) levels a condition which, over time, damages blood vessels, nerves, kidneys, eyes, and the heart.
There are several types, but the two most common are:
- Type 1 diabetes: An autoimmune condition in which the pancreas produces little or no insulin. This form typically requires lifelong insulin therapy.
- Type 2 diabetes: Characterized by insulin resistance (the body does not effectively use its own insulin) or relative insulin deficiency. This is the dominant form in adults.
In African populations, Type 2 diabetes is becoming more prevalent due to factors such as urbanization, dietary change, and increasingly sedentary lifestyles.
Signs and Symptoms
Common signs of diabetes include:
- Excessive thirst (polydipsia)
- Frequent urination (polyuria)
- Increased hunger (polyphagia)
- Unexplained weight loss
- Blurred vision
- Fatigue
These symptoms may appear suddenly in Type 1 diabetes, but in Type 2 diabetes they often develop more gradually.
Complications may already be present by the time someone is diagnosed, because many people with Type 2 diabetes do not notice early symptoms.
Diagnosis and Management
Diagnosis
- Diagnosis usually involves measuring fasting plasma glucose. A fasting blood glucose of 7.0 mmol/L (126 mg/dL) or higher may indicates diabetes.
- Other tests include HbA1c (glycated hemoglobin), which reflects average blood glucose over the prior two to three months, though access to this may be limited in low-resource settings.
Management
Managing diabetes in requires a combination of clinical treatment, regular monitoring, and practical lifestyle changes. Many patients in Africa face structural barriers such as cost, long travel distances to clinics, stockouts of essential medicines, and limited access to specialists. Despite these challenges, well designed care plans can improve outcomes and help prevent long term complications.
Medications
Effective drug therapy remains central to diabetes care.
For Type 1 diabetes, insulin therapy is essential because the body produces little or none of its own insulin. Patients typically use a basal insulin for background control and a rapid acting insulin around meals. In many African countries, human insulin is more commonly available than newer insulin analogues because it is less expensive. However, even human insulin can be difficult to obtain. WHO and Africa CDC reports show that supply interruptions, storage problems, and high retail prices continue to restrict access. Only about half of people with Type 1 diabetes in the region can reliably obtain insulin, which often leads to poor glycemic control and higher risk of diabetic ketoacidosis.
For Type 2 diabetes, treatment usually begins with metformin, a drug that reduces glucose production in the liver and improves insulin sensitivity. Metformin is widely recommended because it is low cost, safe, and effective for most patients. If blood glucose remains above target, clinicians may introduce other oral agents such as sulfonylureas or DPP-4 inhibitors, although availability varies widely by country. When oral therapy no longer maintains blood sugar goals, patients may require basal insulin. In many clinics, the transition to insulin is delayed due to cost barriers, patient fear of injections, or limited health worker training. This delay can lead to neuropathy, kidney injury, or chronic foot ulcers that could have been prevented with earlier intensification of therapy.
Glucose-lowering drugs that protect the heart and kidneys, such as SGLT2 inhibitors or GLP-1 receptor agonists, are rarely accessible in most African settings because of their high cost. Some countries have begun exploring pooled procurement or generic versions, but availability remains uneven as of writing this publication.
Monitoring
Monitoring is just as important as medication. Patients need to track blood glucose trends over time to guide treatment decisions, detect early complications, and adjust diet or activity levels. In practice, however, many households cannot afford test strips, which may cost more than the monthly cost of metformin. As a result, people often rely on occasional clinic checks rather than home monitoring. This pattern can mask dangerous spikes in glucose and delay treatment adjustments.
Routine complication screening is a core part of diabetes care. Foot examinations help detect nerve damage, poor circulation, and early ulcers. Without early detection, small injuries can progress to infections that require amputation. Eye screening for diabetic retinopathy is recommended yearly, but very few facilities have trained ophthalmic staff, and many patients cannot pay for travel to regional hospitals. Kidney screening using urine albumin tests or serum creatinine is also advised, yet access remains inconsistent. These gaps explain why many patients discover complications at an advanced stage.
Lifestyle Changes
Lifestyle modification is the foundation of diabetes care and is critical in African contexts where resources may be limited. A balanced diet is essential but must also be realistic and culturally informed. Patients often rely on staple foods such as cassava, maize, plantain, or rice, which can raise blood glucose when eaten in large portions. Nutrition counselling therefore focuses on portion control, adding vegetables and legumes, reducing sugary beverages, and selecting cooking methods that use less oil. Where nutritionists are scarce, nurses or community health workers often provide basic diet counselling.

Physical activity offers a powerful tool for lowering blood glucose and improving insulin sensitivity. Walking, gardening, farming tasks, and structured community exercise groups all provide accessible options. The goal is usually at least 150 minutes of moderate activity per week, though any increase in movement helps.
Weight management is important for people with Type 2 diabetes. Excess body fat, especially around the abdomen, worsens insulin resistance. Even a modest reduction in weight can improve blood sugar levels and reduce medication needs.
Tobacco avoidance is vital because smoking raises cardiovascular risk, already elevated in people with diabetes. Alcohol moderation is also encouraged because alcohol can cause unstable blood sugar levels and interacts with some medications.
Challenges of Living with Diabetes in Africa
There are numerous barriers that make managing diabetes in Africa particularly difficult:
- High Rates of Undiagnosed Disease
- According to WHO data, only about 46 percent of people with diabetes in Africa know their status.
- Because early-stage diabetes often lacks obvious symptoms, people may not seek testing until complications arise.
- Limited Healthcare Infrastructure
- In many areas there are inadequate testing facilities, few trained health workers, and weak systems for long-term care.
- Clinics are often under-resourced, and many patients miss follow-up appointments.
- Insufficient Access to Medication
- The cost of insulin, monitoring tools, and other drugs is prohibitive for many.
- Insulin supply can be erratic.
- Only a fraction of diagnosed patients achieve glycemic control. For example, studies in primary care settings report target HbA1c (≤ 7%) attainment rates as low as 10–35 percent.
- Socioeconomic and Cultural Barriers
- Low awareness of diabetes contributes to late presentation.
- Poverty makes it hard for patients to afford glucose monitors, test strips, or even travel to clinics.
- In some communities, patients first go to traditional healers, delaying biomedical treatment.
- Health worker shortage and inadequate training limit diabetes education and management.
- Disease Biology and Genetics
- Emerging research suggests that in Black Africans, the pathophysiology of Type 2 diabetes may differ: there may be reduced hepatic insulin clearance and hyperinsulinemia, which contribute to earlier onset and more rapid progression.
- Rapid urbanization, increasing obesity, and dietary shifts are accelerating the burden.
Prognosis & Complications

Without effective treatment, diabetes can lead to:
- Heart attacks and stroke
- Kidney failure (diabetic nephropathy)
- Nerve damage (neuropathy), including foot ulcers and risk of amputation
- Eye disease (retinopathy), which can lead to blindness
Acute presentations such as diabetic ketoacidosis (more common in Type 1) and hyperosmolar hyperglycemic state (in Type 2) carry high mortality when management is delayed or resources are lacking.
In Africa, premature death from diabetes (before age 70) is especially common: WHO reports 58 percent of diabetes-related deaths in the region occur before the age of 70, compared to 48 percent globally.
Lifestyle Modifications: Living Well with Diabetes
Even in resource-limited settings, lifestyle interventions can make a substantial difference:
- Encourage a balanced diet built around local, affordable foods (whole grains, legumes, vegetables), minimizing added sugar and processed foods.
- Promote physical activity adapted to community context (walking, farming, dancing).
- Support education about self-monitoring (where possible), foot care, and recognizing warning signs of complications.
- Foster community networks and peer support to improve adherence, reduce isolation, and share practical strategies.
These modifications not only improve glycemic control but also reduce cardiovascular risk and improve quality of life.
The Way Forward for Africans
Addressing the diabetes crisis in Africa will require coordinated efforts across policy, health systems, and communities:
- Strengthen Screening and Early Diagnosis
- Scale up low-cost screening in primary care.
- Train health workers to recognize early symptoms and risk factors.
- Increase public awareness about diabetes through campaigns and community outreach.
- Improve Access to Essential Medicines and Technologies
- Expand reliable supply of insulin and affordable test strips.
- Promote local production: for example, a recent partnership between a multinational company and a South African facility aims to produce millions of insulin vials for African patients.
- Implement decentralized models of care (e.g., bring diabetes management to district hospitals). The WHO led PEN Plus initiative is an example.
- Strengthen Health Systems
- Train and retain healthcare workers focused on non-communicable diseases.
- Develop chronic care clinics with capacity for follow-up, education, and complication screening.
- Establish patient registries to monitor outcomes and quality of care.
- Policy and Financing
- Governments should allocate more resources toward diabetes care; currently, investment in diabetes in Africa is very low.
- Integrate diabetes into existing non-communicable disease strategies.
- Explore innovative financing models, such as task-shifting, pooled procurement of diabetes supplies, or community-based insurance.
- Research and Innovation
- Support studies that examine the biology of diabetes in African populations (e.g., insulin clearance, beta-cell function).
- Leverage digital health and artificial intelligence to manage care. For instance, AI tools could support diagnosis and monitoring in resource-limited settings.
- Encourage culturally appropriate self-management interventions, including mobile apps tailored to different African contexts and languages.
Living with diabetes mellitus in Africa presents unique challenges—from high rates of undiagnosed disease to limited access to insulin, testing, and long-term care. Nonetheless, through a combination of early detection, affordable treatment, patient education, and health system strengthening, the burden can be reduced. There is a clear need for political will, resource investment, and innovation. By taking these steps, health systems and communities across Africa can better support people with diabetes, reducing complications and improving quality of life.