Residents of Ogijo, a community straddling Lagos and Ogun States, are facing a mounting public health emergency tied to lead poisoning. Recent investigations, blood tests, and soil analyses have revealed widespread contamination linked to informal battery-recycling plants.
Evidence of Contamination in Ogijo
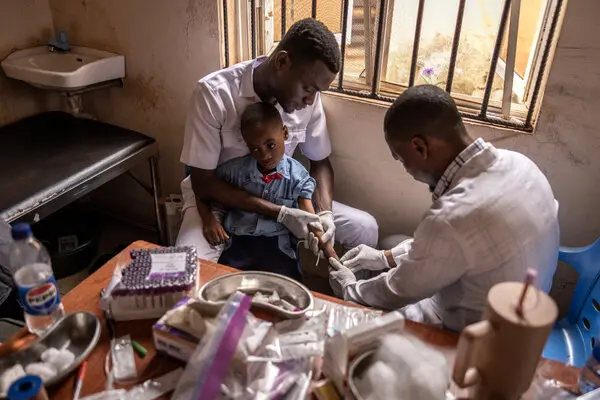
In September 2025, over 70 residents of Ogijo including children and adults — visited the community health centre to collect the results of blood lead level (BLL) tests after months of exposure from nearby battery recycling factories.
Laboratory findings from independent researchers revealed alarming blood lead concentrations. Among factory workers, average BLL hovered around 20 micrograms per decilitre (µg/dL), with some readings as high as 38 µg/dL — well above safety thresholds established by the World Health Organization (WHO).
Children tested also had worrisome levels: average BLL in the cohort was approximately 12 µg/dL, with nearly 75 percent exceeding the WHO reference limit of 5 µg/dL.
In contrast, control samples from individuals living outside the exposure zone typically returned blood lead levels below 0.2 µg/dL.
Environmental sampling painted a grim picture. Soil samples from areas around homes, schools, and play areas occasionally revealed lead concentrations up to 1,901 parts per million (ppm) — frequently surpassing international safety limits for play areas. Dust and slag samples from households and public spaces also often exceeded acceptable thresholds, reflecting chronic environmental contamination.
Investigators attributed the contamination primarily to informal recycling of used lead-acid batteries. When batteries are melted or burned without adequate controls, lead-laden dust, smoke, and slag escape into air, soil, and water exposing nearby residents via inhalation, ingestion of contaminated dust, or consumption of polluted water or food.
Taken together, the data suggest that parts of Ogijo have become hazardous zones with lead levels that pose serious risk to human health.
Health Effects of Lead Poisoning: From Subclinical Harm to Severe Illness
Lead is a potent neurotoxin and systemic poison. Wherever lead dust or contaminated soil is inhaled or ingested, it can accumulate in the bloodstream and deposit in critical organs including the brain, liver, kidneys, and bones. Even low-level chronic exposure can cause long-term damage.
Children are especially vulnerable. Elevated blood-lead levels in childhood correlate with impaired cognitive development, lower intelligence quotient (IQ), learning difficulties, behavioural disorders and even siezures. A report cited by investigators noted that children with BLLs as low as 5 µg/dL scored up to five IQ points lower than unexposed peers.
In adults, lead exposure has been linked to hypertension, kidney damage, reproductive problems, and other chronic health conditions.
The problem is compounded by the fact that there is no known safe level of lead exposure. WHO and global health advocates maintain that even minute amounts of lead can cause harm over time.
In Ogijo, some residents already report symptoms consistent with lead toxicity: abdominal pain, fatigue, reduced concentration, frequent illnesses.
Given the scale of environmental contamination and the proximity of affected populations reportedly more than 20,000 people live within one mile of the recycling plants , the crisis may well extend beyond the few dozen individuals tested.
Response from Authorities and Regulatory Action
The emergence of indisputable data triggered a decisive response. On 26 November 2025, the government announced the shutdown of True Metals Nigeria Limited, one of the key battery-recycling plants responsible for the pollution.
The closure came after regulators found that the company operated under hazardous and dehumanising conditions, and failed to comply with environmental and occupational safety regulations.
At the national level, the Federal Ministry of Health and Social Welfare (FMoHSW) recently inaugurated a National Inter-Agency Working Group on Lead Poisoning Elimination and unveiled a Five-Year Strategic Plan to eliminate lead poisoning across Nigeria.
The initiative aims to scale up blood-lead testing capacity, expand surveillance, enforce regulations across sectors (environment, mining, manufacturing, consumer products), and promote public awareness.
Regulatory agencies have also ramped up scrutiny of consumer products. Recently, collaboration between regulatory bodies and civil society targeted lead contamination in paints, toys, cosmetics, and other everyday items.
These efforts reflect growing recognition at federal and local levels that lead poisoning remains one of Nigeria’s most preventable yet under-addressed environmental health threats.
Challenges to Addressing the Crisis
Despite the regulatory response, multiple hurdles remain before Ogijo and similar communities are truly safe.
First, exposure pathways extend beyond occupational settings. Lead dust persists in soil, water, household dust, and even in reused slag, which residents sometimes repurpose for road filling or land reclamation. This means that even after factory closures, the risk may linger for years.
Second, remediation is complex and costly. Cleaning contaminated soil, demolishing unsafe structures, and ensuring safe waste disposal demand significant resources and technical expertise. Nigeria’s previous lead crises such as the 2010 outbreak in Zamfara State showed that environmental cleanup is arduous and often incomplete.
Third, sustained surveillance and public education are required. The new National Strategy will need funding, political will, and cross-sector collaboration to fully implement blood testing, chelation therapy where needed, and continual monitoring of water, soil, and consumer products.
Finally, the burden of illness is not always obvious. Lead poisoning often progresses silently, with symptoms developing over months or years, especially in children where cognitive effects may not become apparent until school age. This complicates timely diagnosis and intervention.
What Clinicians and Public Health Practitioners Should Know
For health professionals working in Lagos, Ogun, and surrounding regions, the Ogijo crisis offers several lessons and responsibilities.
- Consider lead toxicity in patients especially children who present with developmental delay, behavioural problems, chronic gastrointestinal complaints, or unexplained anemia; particularly if they live or grew up near battery-recycling, smelting, or heavy-industry zones.
- Blood lead testing should be part of diagnostic evaluation where indicated; BLL above 5 µg/dL should prompt environmental assessment and possible intervention.
- For confirmed elevated BLLs, collaborative management may include chelation therapy (depending on severity), but also environmental history and remediation guidance to prevent re-exposure.
- Public health efforts should integrate environmental surveillance, community engagement, and regulatory enforcement. Clinicians can partner with local agencies to report suspected clusters.
- Community education remains vital: raising awareness about lead risks, safe disposal of batteries, avoiding reuse of industrial slag or contaminated soil, using clean water sources, and promoting hygiene to reduce ingestion of dust.
Lead Poisoning in Nigeria
Ogijo is not an isolated case. Nigeria has witnessed mass lead poisoning outbreaks before, notably in Zamfara State (2010) and Niger State (2015), when unsafe mining and ore processing killed or permanently disabled hundreds of children.
Moreover, studies of soil around residential areas in Lagos and Ibadan found elevated lead (and cadmium) levels, especially in low-income settlements, likely from paints, industrial emissions, or historical pollution.
These findings suggest that beyond mining or battery recycling communities, many urban and peri-urban areas may contain hidden lead hazards a national public health burden.
The recent national policy and working group may therefore mark a turning point in Nigeria’s response to environmental heavy-metal exposure.
Frequently Asked Questions
Is there a “safe” level of lead in blood?
No. According to WHO and recent investigations, there is no safe level of lead exposure. Even low blood lead levels as low as 5 µg/dL are associated with harmful effects, especially in children.
What are the common signs of lead poisoning?
In children: developmental delay, learning difficulties, behavioural problems, reduced cognitive performance. In adults: high blood pressure, kidney problems, reproductive issues, fatigue, gastrointestinal discomfort. Chronic exposure can also cause neurological damage over time.
Can lead poisoning be treated?
Yes chelation therapy can help reduce the body’s lead burden in cases of elevated blood-lead levels. However, treatment alone is insufficient without eliminating the source of exposure (contaminated soil, dust, water, air).
What preventive actions can communities take?
Avoid living or raising children near battery-recycling or smelting plants; avoid using industrial slag or contaminated soil for home construction or road filling; use safe water sources for cooking/drinking; wash hands frequently to reduce ingestion of dust; support advocacy for stricter enforcement of environmental and occupational regulations.

