What Is a Stroke
A stroke occurs when blood flow to a part of the brain is interrupted or when a blood vessel in the brain ruptures. This disruption deprives brain cells of oxygen and nutrients, causing them to die.
There are two main types of stroke:
- Ischemic stroke — this is by far the most common, accounting for about 87 percent of all strokes. It happens when a blood clot (or buildup of fatty deposits) blocks an artery supplying the brain, preventing oxygen-rich blood from reaching brain tissue.
- Hemorrhagic stroke — less common, this occurs when a weakened blood vessel ruptures, causing bleeding into or around the brain, which damages brain tissue.
There is also a related condition called a Transient Ischemic Attack (TIA), sometimes referred to as a “mini-stroke.” In a TIA, the blockage is temporary and symptoms resolve within minutes to hours. Although a TIA does not cause permanent brain damage, it is a serious warning sign: many people who have a TIA may go on to experience a full stroke.
How to Identify a Stroke Quickly
Because every minute without treatment can lead to more brain damage, rapid identification of stroke symptoms is critical.
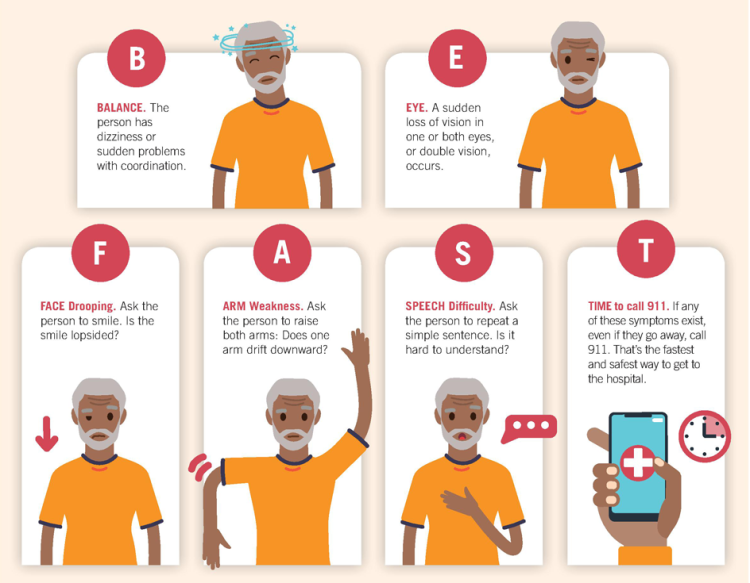
The widely used acronym F.A.S.T. helps people remember the key warning signs:
- Face drooping: Ask the person to smile. Does one side of the face droop or look uneven?
- Arm weakness: Ask them to raise both arms. Does one arm drift downward or feel weak?
- Speech difficulty: Is speech slurred or odd? Ask the person to repeat a simple sentence. Can they do it correctly?
- Time to call emergency services: If you see any of these signs, call immediately and note the time when symptoms began.
Because some strokes particularly those affecting the back of the brain, may present with symptoms that F.A.S.T. does not capture, some health-education campaigns use an extended mnemonic: B.E. F.A.S.T., adding Balance (sudden dizziness or loss of balance) and Eyes (sudden trouble seeing).
Other possible signs beyond F.A.S.T include: sudden confusion, trouble understanding speech, sudden vision changes, difficulty walking or coordination problems, unprovoked sudden severe headache, or sudden numbness/weakness in the leg.
Because strokes can unfold in diverse ways and sometimes subtly especially in women, any abrupt neurological change should prompt immediate evaluation.
What to Do Immediately if You Suspect a Stroke
In most African settings, rapid access to ambulance services varies by region. Some communities have well equipped emergency medical systems, while others rely on family members, neighbours or local transport. Regardless of location, fast action is essential because brain cells begin to die within minutes.
If stroke symptoms appear, call your local emergency number if an ambulance service is available in your area. In places where emergency response is limited, arrange the fastest safe transport to the nearest health facility that can perform brain imaging. This is important because treatment depends on whether the stroke is caused by a clot or bleeding.
If you are supporting someone with suspected stroke, note the time symptoms started or the last time the person was seen well. This helps clinicians decide whether clot-dissolving therapy or mechanical clot removal is possible.
Keep the person calm and comfortable while arranging transport. If they are conscious, help them lie on their side with the head slightly raised. If they are unconscious or fell, avoid moving them unless they are in danger.
Do not give food, drinks, or any medicines before reaching a facility. Stroke often affects swallowing and increases the risk of choking. Giving aspirin is risky because it can worsen bleeding in the case of a hemorrhagic stroke.
Diagnosis, Treatment, and After-care
Once the patient reaches a hospital, clinicians will perform brain imaging (usually a non-contrast computed tomography CT scan) as quickly as possible. This helps distinguish between ischemic and hemorrhagic stroke and determine appropriate treatment.
For ischemic stroke (caused by a clot), when treatment begins early enough, there are powerful interventions:
- Intravenous thrombolysis with a drug such as recombinant tissue plasminogen activator (rtPA) remains the standard if started within 4.5 hours of symptom onset (assuming no contraindications).
- Mechanical thrombectomy, an endovascular procedure to physically remove the clot, can benefit patients with large vessel occlusion. In eligible patients, thrombectomy ideally occurs within 6 hours; but updated guidelines allow treatment up to 24 hours in select cases with appropriate imaging and favorable findings.
For strokes caused by bleeding (hemorrhagic), the treatment is different: doctors focus on controlling bleeding and intracranial pressure, normalizing blood pressure, and sometimes surgical intervention.
In the case of a TIA, even if symptoms resolve quickly, urgent evaluation is critical. Imaging and tests help identify the cause, such as narrowed arteries or heart rhythm disorders. Even though TIAs often leave no permanent damage, roughly one-third of individuals who have a TIA may have a full stroke eventually.
A long-term study showed that among people who had a TIA or minor stroke, nearly 6 percent had another stroke within one year, and almost 20 percent within ten years , showing the need for sustained prevention.

Why Rapid Action Matters
Brain tissue is highly vulnerable to oxygen deprivation. In untreated stroke, nerve cells begin to die within minutes.
Delays reduce the chance that clot-busting or clot-removing treatments will work. For clot-based (ischemic) stroke, the “therapeutic window” is narrow: ideally within 4.5 hours for thrombolysis, and within 6 to 24 hours for thrombectomy (depending on imaging and individual criteria) for eligible patients.
After that window, treatment options are more limited and the risk of long-term impairment or death rises significantly. This is why first responders and hospitals aim to minimize the time from symptom onset to diagnosis and treatment.
Risk Factors for Stroke in Africa
In Africa, many of the risk factors for stroke match those described globally; but patterns of prevalence and impact differ, partly because of varying socio-economic conditions, health-care access, lifestyle shifts and population demographics.
Here are the major risk factors for stroke:
Non-modifiable risk factors
- Age: As worldwide, advancing age increases stroke risk. In Africa, though, strokes often occur at younger ages compared to high-income countries. For example, some African cohorts report mean age of stroke onset around 57–59 years versus ~66 years elsewhere.
- Sex, heredity and genetic traits: Gender, inherited cardiovascular risk, family history of stroke or prior transient ischaemic attack (TIA) contribute.
Modifiable risk factors (behavioral, metabolic, health conditions, environment)
- High blood pressure (hypertension): This is the single most powerful risk factor for stroke across Africa. Several studies find that up to 90% of stroke risk in certain populations is attributable to hypertension. Many African countries have rising hypertension prevalence related to urbanization, changing diets, and limited blood pressure screening and control.
- Diabetes mellitus (type 2 diabetes): Elevated blood glucose increases stroke risk. In Africa rising rates of diabetes especially in urban areas raise concerns about future stroke burden.
- Dyslipidaemia (abnormal blood lipids): High cholesterol or abnormal blood fat levels, particularly elevated low-density lipoprotein (LDL), contribute to stroke risk across many African regions.
- Obesity and central obesity (abdominal fat): Obesity and increased waist-hip ratio increase risk of stroke by promoting hypertension, diabetes, dyslipidaemia, and other metabolic disturbances.
- Physical inactivity, unhealthy diet and lifestyle changes: Urbanization, shifting diets (higher salt, processed foods, saturated fats), lower consumption of vegetables, and reduced physical activity all fuel the rise in metabolic and vascular risk factors.
- Tobacco use (smoking) and harmful alcohol intake: Smoking increases risk for all types of stroke. Alcohol intake also contributes, especially to hemorrhagic stroke, although data vary by region.
- Cardiac disease (heart disease, heart rhythm disorders, heart valve disease): Conditions such as cardiomyopathy, arrhythmias, atrial fibrillation, and other heart diseases raise stroke risk especially for ischaemic stroke.
- Prior transient ischaemic attack (TIA) or previous stroke: History of TIA or stroke raises the chance of future stroke events.
Frequently Asked Questions (FAQ)
What is the difference between a stroke and a TIA?
A stroke involves a prolonged interruption of blood supply or bleeding that causes irreversible brain injury. A TIA (transient ischemic attack) is a short-lived blockage symptoms typically resolve within minutes to hours and often leave no permanent damage. However, a TIA is a serious warning sign that a full stroke might follow.
Why is “time of onset” so important?
Certain treatments like intravenous clot-dissolving drugs are only effective if started within a limited time window (up to 4.5 hours for most patients). For mechanical clot removal, some eligible patients may benefit up to 24 hours after onset but only if imaging shows salvageable brain tissue.
Is it safe to give a suspected stroke patient aspirin or water?
No. You should not give food, drink, or medications such as aspirin, because you do not yet know whether the stroke is caused by clot or bleeding. Treat it as an emergency and wait for trained medical professionals.
Can people recover fully from stroke?
Yes — especially if treatment happens early. But recovery depends on many factors: type of stroke, how quickly care started, the brain area affected, and how promptly risk factors are managed. Rehabilitation (physical, speech, occupational therapy) often plays a key role.
How can I reduce my risk of stroke?
Focus on controlling modifiable risk factors: keep blood pressure, blood sugar, and cholesterol in check; stay physically active; eat a balanced diet; avoid smoking; limit alcohol; and attend regular medical checkups. For people who had a TIA or prior stroke, taking prescribed antiplatelet or anticoagulant medications, and following lifestyle recommendations, dramatically lowers the risk of another stroke.
** This Article has been Reviewed by Dr. Chimaobi Felix, MBBS
⚕ Medical Disclaimer
This article is for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making any health decisions. The Healthy African is not liable for any actions taken based on the information provided on this site.

