Fake or substandard medicines are a serious health risk across much of Africa. When someone takes a counterfeit drug—one that is falsified, lacks the correct active ingredients, has too much or too little of them, or is contaminated—the consequences for the liver, kidneys, digestive tract, skin, and other systems can be severe.
A real story: when fake medicine almost claimed a life
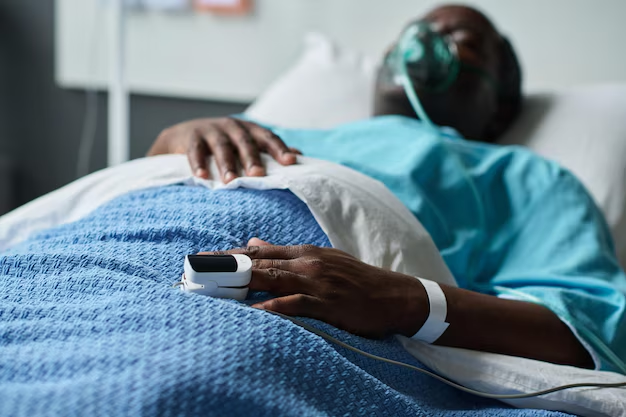
A close friend of mine recently fell gravely ill after taking what he believed was a reputable antimalarial medicine. Within hours of completing the course, he began to feel extremely weak. His legs could no longer support him, and he collapsed at home. He was rushed to the hospital, where doctors immediately ran several tests, including liver and kidney function panels.
The results showed that his liver enzymes were dangerously elevated, a clear indication of acute liver injury. The medication he had used turned out to be counterfeit—its contents did not match what was stated on the label. The toxic compounds inside were actively destroying his liver cells. Physicians started him on intensive treatment, including intravenous fluids, detoxification support, and liver-protective therapy.
Fortunately, his condition improved after several days of hospital care. But the doctors warned that had he delayed coming to the hospital, he could have lost his life. His experience is a reminder that fake medicines are not just ineffective—they can be deadly within days.
Why fake drugs are so common in Africa

Recent studies show that about 22.6% of medicines tested across Africa are substandard or falsified, meaning they failed at least one quality test
Several factors drive this crisis:
- Weak regulatory oversight and limited enforcement in some countries.
- High medication demand combined with poverty and inadequate access to formal pharmacies.
- Complex supply chains with multiple intermediaries that allow low-quality or counterfeit products to infiltrate.
- Growth of online and informal street markets where medicines are sold without registration or verification.
How fake medications harm the body
The damage depends on the defect in the drug—whether it contains no active ingredient, the wrong dose, or toxic contaminants such as mercury, arsenic, or industrial solvents .
Liver
- Early symptoms: nausea, vomiting, jaundice (yellowing of skin or eyes), mild pain under the right rib (where liver is located), dark urine.
- Late symptoms: acute hepatitis, elevated liver enzymes, possibility of liver failure, cirrhosis if damage persists, increased risk of drug-induced liver injury.
Kidneys
- Early symptoms: reduced urine output, swelling (especially legs, ankles), fatigue, dark or foamy urine.
- Late symptoms: acute kidney injury (AKI), chronic kidney disease (CKD), dialysis may become necessary if kidneys fail.
Gastrointestinal system
- Early symptoms: abdominal pain, nausea, vomiting, diarrhea, possibly bleeding, or gastrointestinal irritation.
- Late symptoms: malabsorption, ulceration, chronic gastritis or enteritis, gut flora imbalance, digestive enzyme deficiencies.
Skin
- Early symptoms: rash, itching (pruritus), hives, discoloration.
- Late symptoms: severe reactions like Stevens-Johnson syndrome or toxic epidermal necrolysis (rare but serious), scarring, permanent pigmentation changes.
Other possible effects include immune reactions, allergy, systemic poisoning from heavy metals, or organ-toxicity from undeclared chemicals. Fake antibiotics or antimalarials may lead to treatment failure and drug resistance.
What to do if you suspect you have taken a fake medicine
- Stop taking the drug immediately and keep any remaining tablets or packaging. These can help doctors and investigators identify the product.
- Seek medical attention quickly. Bring the medicine and packaging to the hospital and explain when and where you purchased it.
- Expect laboratory tests, including liver function (ALT, AST, bilirubin), kidney function (creatinine, urea), and electrolytes.
- Treatment may include fluids, detoxification, liver-protective medications, or dialysis if the kidneys are affected.
- Report the case to your country’s drug regulatory agency (for example, NAFDAC in Nigeria). Reporting helps identify counterfeit batches and protect others.
If my friend’s case shows anything, it is that swift medical action can be life-saving. The doctors said his timely arrival at the emergency department prevented complete liver failure.
Prognosis
With early treatment, organ damage may reverse. However, severe liver or kidney injury can cause permanent impairment. Delayed medical care increases the risk of death or chronic illness.
How to identify fake medicines in the future
Identifying fake medications is very important in avoiding the damage to health consuming them comes with, In another article I explained how you can carefully identify fake medications, read here.
Frequently asked questions (FAQ)
Q: Can fake medicines ever be safe if taken in small quantities?
A: No. Even small amounts can contain toxic contaminants or unpredictable doses.
Q: I took a fake medicine but feel fine. Should I still see a doctor?
A: Yes. Liver or kidney damage can progress silently for days or weeks before symptoms appear.
Q: Are herbal or “natural” products safer?
A: Not necessarily. Herbal preparations can also be falsified or contaminated with heavy metals or synthetic drugs.
Q: What can health authorities do to curb fake drugs?
A: Enforce stricter regulation, monitor supply chains, expand authentication systems, and educate the public and healthcare providers.
Fake medications continue to threaten lives across Africa. My friend’s experience illustrates how quickly a routine illness can turn into a medical emergency when counterfeit drugs are involved. Awareness, vigilance, and rapid response remain the best protection. Patients must report suspicious medicines, while healthcare workers should advocate for stronger regulation and patient education.
No one should lose their life to a fake pill. Early recognition and decisive medical care can make the difference between recovery and tragedy.
