Your kidneys do more work than most people realize. These two bean-shaped organs, each roughly the size of a fist and tucked just below your rib cage on either side of your spine, filter about 200 liters of blood every day. They flush out waste, regulate blood pressure, balance salt and fluid levels, and produce hormones that keep your bones strong and your red blood cells healthy. When they stop working, everything falls apart – and the consequences can be fatal without medical intervention.
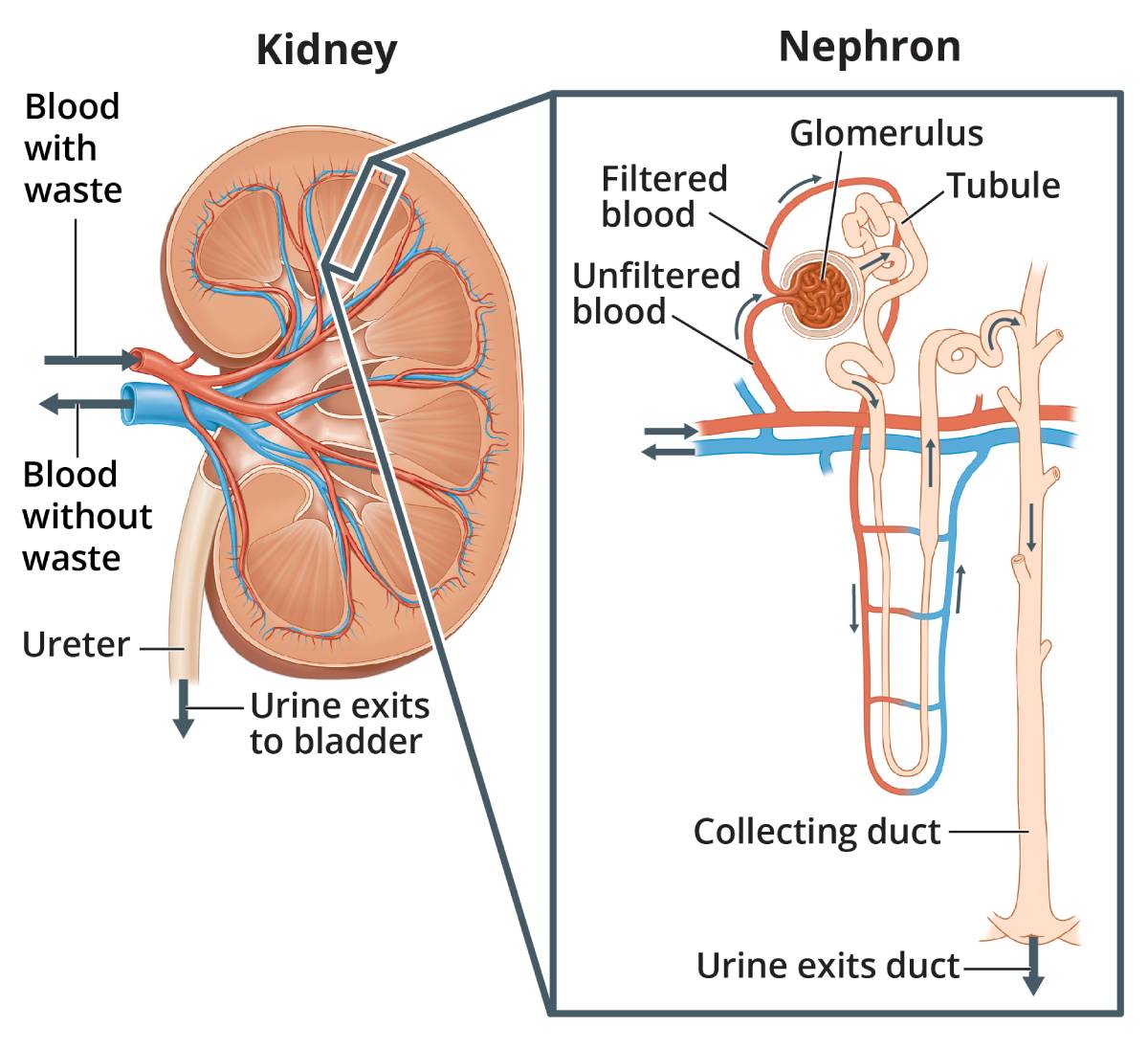
Kidney failure, also called renal failure or end-stage renal disease (ESRD), is the point at which the kidneys have lost so much function that they can no longer keep a person alive on their own. When kidney failure occurs, the kidneys have lost 85 to 90 percent of their normal function, and treatment with dialysis or a kidney transplant becomes necessary.
What Exactly Happens When Kidneys Fail?
Kidney failure does not happen overnight in most cases. It is usually the final stage of a long, gradual process called chronic kidney disease (CKD). Think of CKD as a slow leak in a tire: the tire keeps rolling for a while, but it eventually goes flat. There are two broad types of kidney failure: acute kidney failure, which develops quickly and may be reversible, and chronic kidney failure, which results from damage that builds up slowly and cannot be reversed.
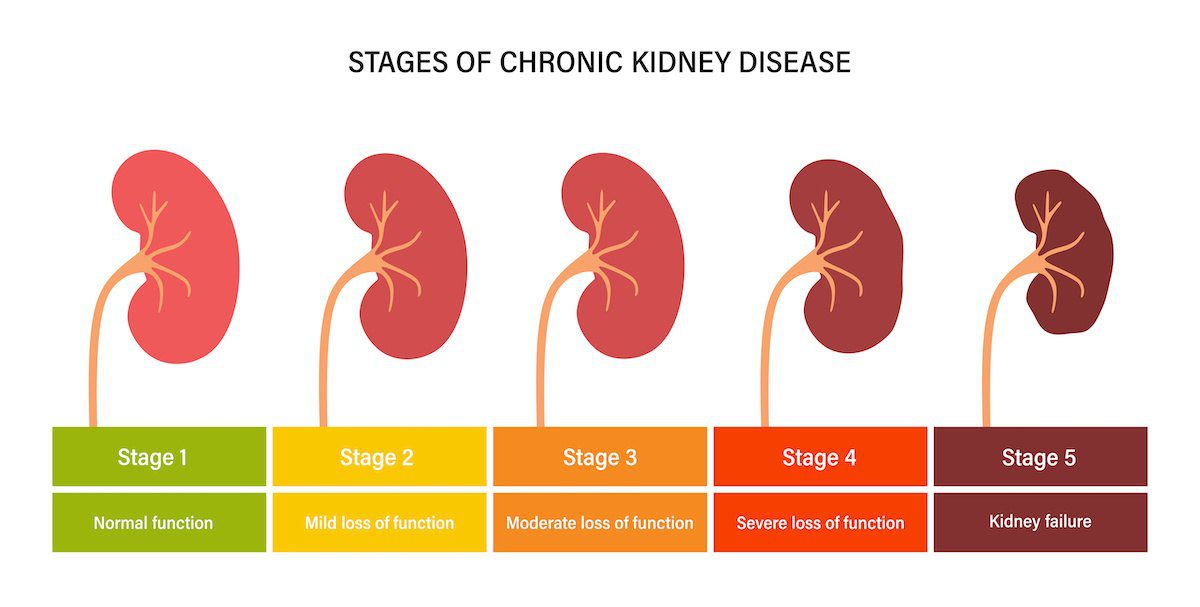
When kidneys fail, waste products, excess fluids, and toxins accumulate in the blood – a condition called uremia, from the Latin for “urine in the blood.” The body’s chemical balance collapses: sodium, potassium, and phosphorus levels swing out of control; blood pressure climbs; and anemia develops because the kidneys can no longer produce enough erythropoietin, the hormone that triggers red blood cell production.
Common Causes Worldwide
Diabetes and high blood pressure are the two most common causes of kidney failure globally. (Cleveland Clinic, March 2026) Together, they account for the majority of new kidney failure cases in most countries.
In diabetes, persistently high blood sugar damages the tiny blood vessel clusters called glomeruli – the kidney’s microscopic filters. The hyperglycemia of diabetes damages the kidneys through several mechanisms, including increased capillary pressure that causes structural changes in the glomerulus, leading to a thickened basement membrane, an enlarged mesangium, and eventually fibrosis. Fibrosis means permanent scarring, and scarred kidneys cannot regenerate.
Diabetes is the leading cause of kidney failure globally, and in many countries, half of all people starting dialysis have kidney failure caused by diabetes. (World Kidney Day 2026)
High blood pressure forces the kidneys to work under constant excess strain. Over time, it damages both the glomeruli and the blood vessels that supply them. Other global causes include:
- Glomerulonephritis (inflammation of the kidney’s filtering units)
- Polycystic kidney disease (an inherited condition in which fluid-filled cysts replace normal kidney tissue)
- Repeated urinary tract and kidney infections (pyelonephritis)
- Prolonged use of non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and diclofenac
- HIV-associated nephropathy
- Obstruction from kidney stones or an enlarged prostate
The African Context: A Different and Harder Story
The kidney disease burden in Africa carries distinctive features that set it apart from patterns in high-income countries. In sub-Saharan Africa, the rising prevalence of kidney disease is driven by the combined effects of hypertension, diabetes, and HIV, and by the influence of apolipoprotein L1 (APOL1) genetic variants that increase susceptibility to chronic kidney disease. The APOL1 gene, more common in people of West African ancestry, confers protection against certain parasitic infections but also raises the risk of kidney damage.
In a large cross-sectional study involving more than 8,000 participants from six centers across four African countries, the overall prevalence of chronic kidney disease was reported at 10.7 percent.
Beyond genetics, neglected tropical diseases affecting some of the poorest populations in Africa are also thought to contribute substantially to the chronic kidney disease burden in the region. (Wiley Nephrology – CKD in Africa, 2024) Chronic infections from organisms like schistosomes and malaria parasites can directly injure kidney tissue over years.
One factor that is often overlooked is the widespread use of traditional herbal remedies. The World Health Organization (WHO) estimates that 80 percent of the population in many African and Asian countries rely on herbal medicine for some aspect of primary healthcare. (Indian Journal of Nephrology, 2025) While many herbal preparations are harmless, some contain compounds that are directly toxic to kidney cells. Acute kidney failure from herbal remedies accounts for approximately 30 to 35 percent of all acute kidney failure cases in parts of Africa. (PMC – Acute Renal Failure and Herbal Medicines in Nigeria, 2015) This is a serious, preventable problem that receives too little attention. If you use traditional herbal treatments, always inform your doctor.
The prevalence of treated kidney failure is over 200 times higher in high-income countries than in low-income countries. meaning many Africans with treatable kidney failure never receive the care they need.
Early Signs and Symptoms: The “Silent Killer” Problem
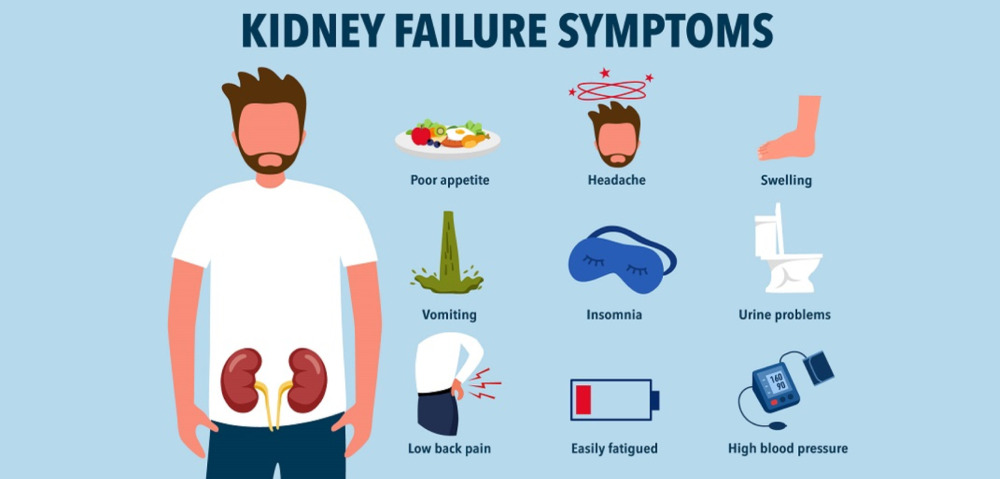
Early chronic kidney disease has no signs or symptoms. (World Kidney Day 2026) This is what makes it so dangerous. Most people feel completely well while their kidney function quietly declines, and by the time symptoms appear, the damage is often severe.
That said, certain signs – especially when they appear together – should prompt an immediate visit to a doctor:
Changes in urination. Producing less urine than usual, or needing to urinate more frequently at night (a symptom called nocturia), is often one of the first clues. Urine may appear foamy, indicating protein leakage, or dark and blood-tinged.
Swelling (edema). When the kidneys cannot remove excess fluid, it pools in the legs, ankles, feet, and sometimes the face or hands. When the kidneys fail to remove excess fluid from the body, it results in swelling in the extremities – known as edema – and is a common symptom of kidney failure. (Apollo Pharmacy Health Blog, 2024)
Fatigue and weakness. When the kidneys are not functioning properly, the resulting buildup of waste products in the blood can lead to constant tiredness and a lack of energy. (Apollo Pharmacy Health Blog, 2024) This is often mistaken for overwork or stress.
High blood pressure that is hard to control. Because the kidneys regulate blood pressure through hormones and fluid balance, damaged kidneys often drive blood pressure upward – creating a cycle where high blood pressure causes more kidney damage.
Shortness of breath. Fluid accumulates in the lungs as kidney function deteriorates, causing breathlessness even at rest. This can occur due to the buildup of fluids in the lungs, a common complication of kidney failure, and may be accompanied by a cough or difficulty breathing. (Apollo Pharmacy Health Blog, 2024)
Nausea, vomiting, and loss of appetite. Uremic toxins in the blood irritate the digestive system. A persistent metallic or ammonia-like taste in the mouth is a particularly telling sign.
Brain fog and confusion. When kidneys stop working properly, symptoms include fatigue, nausea, vomiting, swelling, reduced urine output, and brain fog. (Cleveland Clinic, March 2026)
Itchy, dry skin. When kidneys can no longer maintain the right balance of minerals and nutrients in the blood, the skin can become dry and intensely itchy.
Muscle cramps. Imbalances in electrolytes like calcium and phosphorus, as well as poor blood flow, can lead to persistent muscle cramping.
A 2026 study from Karolinska Institutet, published in Kidney International, found that small changes in kidney function, even when test results fall within what doctors consider a normal range, may reveal who is likely to develop chronic kidney disease later in life.
How Kidney Failure Is Diagnosed
The main diagnostic tests include a blood test measuring estimated glomerular filtration rate (eGFR) – which shows how well the kidneys are filtering blood – and a urine albumin-to-creatinine ratio (uACR) test, which checks for protein that should not normally appear in urine. Imaging tests such as ultrasound and CT scans can detect kidney stones, polycystic kidney disease, and structural abnormalities. (Dialyze Direct, December 2025) A kidney biopsy may be needed in some cases to determine the precise cause of damage.
Treatment Options
Once kidney failure is established, management focuses on keeping the person alive and maintaining quality of life. The two main options are dialysis and kidney transplantation.
Dialysis comes in two forms: hemodialysis, where blood is pumped out of the body, filtered through a machine, and returned (typically three sessions per week); and peritoneal dialysis, where a cleansing fluid is introduced into the abdominal cavity, allowed to absorb waste, and then drained. Whether kidney failure develops gradually or suddenly, it means the kidneys have stopped working well enough to keep a person alive, and dialysis or a transplant becomes necessary.
For patients with diabetic kidney disease, the 2024 KDIGO clinical practice guidelines recommend treatment with a sodium-glucose cotransporter-2 (SGLT2) inhibitor for patients with type 2 diabetes, chronic kidney disease, and an eGFR of at least 20 mL/min per 1.73 m2,News) as these drugs have demonstrated the ability to slow kidney disease progression.
How to Protect Your Kidneys
Many causes of kidney failure are preventable. These are the most evidence-backed protective steps:
- Control blood pressure. Keep it at or below 130/80 mmHg. This single intervention may do more to preserve kidney function than any other measure.
- Manage blood sugar. If you have diabetes, tight blood glucose control substantially reduces the risk of kidney damage. Regular HbA1c monitoring is essential.
- Stay hydrated, but sensibly. Drinking enough water helps the kidneys flush out waste and may help prevent kidney stones and infections.
- Use painkillers carefully. Taking too much of certain pain relievers called NSAIDs, such as ibuprofen or naproxen, can damage the kidneys; safer options should be discussed with a healthcare professional if pain relief is needed frequently.
- Eat less salt and processed food. A low-sodium diet reduces blood pressure and eases the burden on kidney filters.
- Avoid unregulated herbal remedies. Given the documented link between some traditional herbal medicines and kidney damage, always tell your doctor or nurse every preparation you are taking.
- Get routine kidney screening. People with diabetes, hypertension, a family history of kidney disease, obesity, or HIV should have annual eGFR and uACR tests even when they feel perfectly well. Slowing chronic kidney disease progression at early stages provides both economic benefits and prevents the development of kidney failure and cardiovascular complications. (KDIGO 2024 Clinical Practice Guidelines, Kidney International)
- Do not smoke. Smoking constricts blood vessels, worsens hypertension, and accelerates kidney damage.
- Maintain a healthy weight. Being overweight raises the risk of developing diabetes, cardiovascular disease, hypertension, and kidney disease.
Go to a Doctor Immediately If You Notice:
- A sudden, sharp drop in urine output, or no urine at all
- Severe swelling of the face, legs, or abdomen that appears rapidly
- Shortness of breath at rest, or difficulty lying flat
- Confusion, extreme drowsiness, or difficulty staying awake
- Persistent vomiting combined with reduced urination
- Chest pain or irregular heartbeat alongside any of the above symptoms
These signs can indicate acute kidney failure, which is a medical emergency. Do not wait and see – go to the nearest hospital emergency department immediately.
Frequently Asked Questions (FAQ)
Can kidney failure be reversed? Acute kidney failure can sometimes be reversed if the cause is identified and treated promptly, before permanent damage occurs. Chronic kidney failure cannot be reversed; treatment focuses on slowing its progression and managing symptoms.
Can you live a normal life on dialysis? Many people do, though dialysis is demanding. Most patients on hemodialysis attend three sessions per week, each lasting three to five hours. Dietary restrictions and some lifestyle adjustments are necessary, but with good support, work and daily activities remain possible.
Is kidney disease hereditary? Some forms are, including polycystic kidney disease and certain glomerular diseases. The APOL1 gene variant, more common in people of African descent, also confers elevated kidney disease risk. A family history of kidney failure warrants early and regular screening.
What foods are hardest on the kidneys? High-sodium foods such as processed meats, canned soups, and salty snacks; excessive red meat; and in advanced kidney disease, foods high in potassium or phosphorus all place extra strain on the kidneys. Consult a registered dietitian with nephrology experience for personalized dietary guidance.
Can herbal medicines cause kidney failure? Yes. Some herbal preparations contain compounds – including aristolochic acid and atractyloside – that are directly toxic to kidney tubule cells. The risk is particularly well-documented in Africa and Asia. Always inform your doctor about any herbal preparations you take.
What is the difference between CKD and kidney failure? Chronic kidney disease (CKD) describes a spectrum of declining kidney function across five stages. Kidney failure is Stage 5, when the kidneys are functioning at less than 15 percent of normal capacity and life cannot be sustained without dialysis or a transplant.
How do I know if I have kidney disease when there are no symptoms? A simple blood test for eGFR and a urine test for albumin (uACR) can detect kidney problems years before symptoms appear. If you have diabetes, high blood pressure, obesity, or a family history of kidney disease, ask your doctor for these tests annually.
** This Article has been Reviewed by Dr. Chimaobi Felix, MBBS
⚕ Medical Disclaimer
This article is for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making any health decisions. The Healthy African is not liable for any actions taken based on the information provided on this site.
